In the past, doctors dip their hands into chemical solutions, such as potassium, chlorine, or acid to assure hand hygiene before invasive medical procedures. Undoubtedly, this sanitizing method was detrimental to their hands. The invention of sterile gloves completely changed healthcare workers’ approaches to infection. Hygiene in multiple medical fields was taken to the next level.
In the modern world, sterile gloves, also known as surgical gloves, are widely used in hospitals, veterinary clinics, and even beauty salons. It is so popular that many people use them in unnecessary situations. However, the misuse of gloves is a waste of resources and can significantly increase the risk of contamination.
So, when should sterile gloves be worn? In short, sterile gloves are compulsory only in surgical interventions and invasive contact with the human body. Besides learning when to wear sterile gloves, knowing when not to wear them is just as important. Dive in for more details!
Table of Contents
What Are Sterile Gloves
Sterile gloves are a type of disposable rubber gloves. Manufacturers put them through specific procedures to eliminate germs and microorganisms. Some common sterilization methods are ethylene oxide, dry heat, high-pressure saturated steam, and radiation. These are quite similar to the process nurses carry out to prepare a surgical room in the hospital.
Be careful when purchasing sterile gloves. There are two types of medical gloves: non-sterile and sterile. Though their manufacturing process is the same, non-sterile gloves haven’t been sterilized and went through less rigorous quality control. Also, products that are marked as partially sterilized are not surgical gloves.
All sterile gloves in the market must meet the FDA standards. Firstly, the manufacturers acquire the FDA-approved sterile techniques. After the glove production, they will apply those exact techniques to sterilize them. In addition, they have to perform testing procedures before and after production in correspondence to some requirements on materials, incubation conditions, acceptable quality level (from 1.0 to 1.5 for sterilized gloves), dimension test for sufficient thickness, and heat test for resilience.
When You Should Wear Sterile Gloves
As stated in the Glove Use Information Leaflet by WHO, the two main reasons for wearing medical gloves are:
- To lower the risk of contamination to the caregivers when their hands are exposed directly to blood and other bodily fluids.
- To reduce the risk of germs spreading to the environment or from one patient to another or the caregiver to the patient and vice versa.
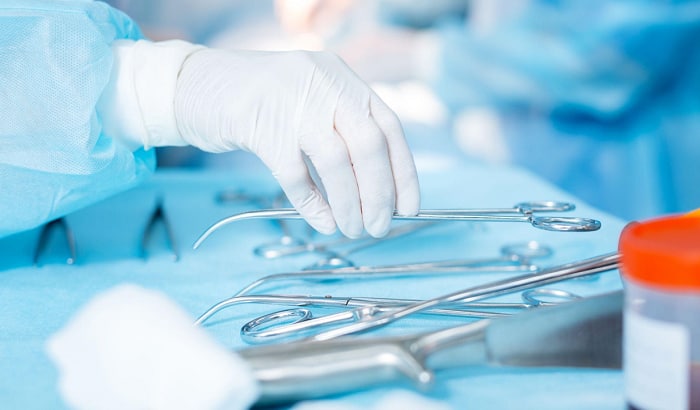
Medical gloves should be used during all patient-care activities that involve coming into touch with blood, bodily fluids, or tissues. When such activities require touching a sterile spot, disposable sterile gloves are needed. In other words, they are required in all surgical interventions and invasive contact with the human body. Sterile latex gloves are usually used for:
- A surgical procedure
- Handling sterilized tools in surgical rooms
- A vaginal delivery (such as delivering a baby)
- An invasive radiological or vascular procedure
- Preparing total parenteral nutrition and chemotherapeutic agents
- Performing dialysis
The contribution of sterile gloves in reducing pathogen transmission is undeniable. However, please note that they do not provide complete protection against all hand contamination. As mentioned above, the acceptable quality level of sterile gloves is 1.0 to 1.5, which means from 1% to 1.5% of sterile gloves in the market might have tiny pinholes.
In addition, applying and removing gloves improperly increases the risk of contamination. Though the probability is low, bacteria can gain access to the healthcare workers’ hands through these small defects. It is vital to wash and rub your hands appropriately before and after donning sterile gloves. Surgical gloves are no substitute to hand hygiene. Always follow these rules:
- Never wear the same gloves for more than one patient. If you take care of one patient for a prolonged period, consider performing hand hygiene and changing gloves in between episodes of care for that patient.
- Hand rub, wash, and dry before putting on sterile gloves and after taking off the gloves.
- If a glove’s integrity is compromised during any procedure (e.g., punctures, splits), immediately remove the gloves and wash your hands.
When Not to Wear Sterile Gloves
Now, you know when to use sterile gloves in nursing. But to put an end to glove wastage and contamination possibility, it is also crucial to learn when not to use them. The misuse of surgical gloves is usually due to inappropriate storage and improper moments.
- Inappropriate storage
In general, disposable sterile gloves have a shelf life of five years when stored in suitable conditions. The storage environment must be cool and dry with a temperature ranging from 50° to 72° F (10°-22° C). Sterile gloves can’t be near heat, humidity, ultraviolet light, radiation, ozone, chemicals, or any other extreme conditions.
Before use, they should always be checked for signs of defects. Gloves that pass their shelf life or look damaged must not be used. Ripped packages mean that the gloves are no longer sterilized, continuing to use them puts both caregivers and patients at high risk of infection. Damaged gloves should immediately be disposed of.
- Wrong moments
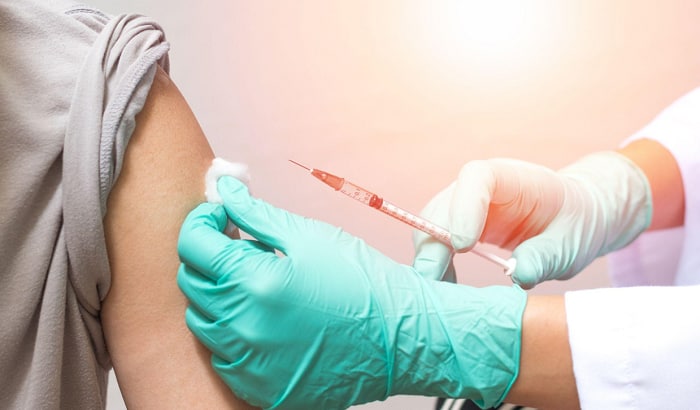
Don’t use sterile gloves when not required. In clinical situations, when there is a potential for touching blood, bodily fluids, tissue, items soiled by blood but no chances of invasive contact with the human body, surgical gloves are not necessary. Here is a list of where examination gloves should be used instead of sterile ones:
- Drawing blood
- Vaccine injections
- Pelvic examination
- Emergencies
- Contact with mucous membrane and non-intact skin
- Potential presence of infectious and dangerous pathogens
- Indirect patient exposure, such as cleaning spills and blood or handling waste
Additionally, activities that happen in contaminated environments and have no potential for blood and body fluid exposure do not require wearing gloves. Don’t put on medical gloves when taking blood pressure, transporting patients, caring for eyes and ears (without contact with secretions), or placing non-invasive ventilation equipment, except for when contact precautions are needed.
Healthcare workers should be trained on how to optimize the use of one glove, as well as change the glove, or apply double-gloving in appropriate practices. Improper applying and removing sterile glove techniques make them a source of contamination.
Steps to Don and Take Off Sterile Gloves Appropriately
Here is how to don sterile gloves.
- Step 1: Take off all jewelry from your hands. Avoid wearing artificial or long nails and nail polish. Also, fold your sleeves up or wear a short-sleeved shirt.
- Step 2: Wash your hands thoroughly with a surgical hand scrub. If there is any wound, cover it. Your hands must be free from all kinds of open lesions and skin fractures.
- Step 3: There should be a clean surface for opening sterile glove packages. Place the package on the table, check if it is intact and not expired. Make sure there are no signs of tears or splits.
- Step 4: Pick up the package and peel it open. Sterile gloves are usually double-packaged.
- Step 5: When you get to the second package, don’t touch the inside because it is sterilized. Instead, pull the edges on the outside to open.
- Step 6: When packaging sterile gloves, manufacturers always fold the cuffs to reveal the inside so that you don’t touch the outside when donning sterile gloves. With your non-dominant hand, pick up the other glove and slide your dominant hand in. Don’t try to unfold the cuff with your bare hand, leave it there.
- Step 7: With your gloved hand, lift the other glove and slide your non-dominant hand in. This time, don’t touch the inside of the folded cuff. Remember that the outside is sterilized while the inside is not because it comes in contact with your skin. Only a sterilized surface should touch another sterilized surface. When both gloves are on, feel free to adjust the fingers.
When you finish the task, take off the gloves and follow these steps.
- Step 1: With your dominant hand, grab the outside of the other glove and slowly pull it off. Allow it to fold inside out so your hand doesn’t contact the outside. Ball the glove up and hold it in your dominant hand.
- Step 2: Slide two fingers underneath the cuff of the glove on your non-dominant hand and gently pull it off from the inside out, wrapping the other glove in it.
- Step 3: All is done. Dispose of the gloves in a proper place.
For visualization, you can watch this video Applying and Removing Sterile Gloves by Ben Meinking.
Conclusion
In conclusion, sterile gloves are an incredible instrument for the reduction of microorganism transmission between caregivers and patients. However, they are only effective when worn properly. Learning when to wear surgical gloves is the first step to absolute medical hygiene.
If you found this article on when should sterile gloves be worn informative, please help us share it with your friends and colleagues who are in need. Before you leave, feel free to let us know should you have any further questions. We are delighted to assist. Thank you for your attention.

Veronica is our content editor. She is a talent in delivery. Her main work is editing and writing articles that are both informative and simple to follow. She is in charge of synthesizing our understanding of what personal protection equipment (PPE) is needed in each job, how to best apply it, and how to visualize that equipment.